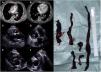
We present a 57-year-old man with history of colon cancer resected in currently chemotherapy treatment because of pulmonary metastases. He consulted to the Emergency Department complaining of acute dyspnoea. Acute pulmonary embolism (PE) was diagnosed by a computed tomography scan (Fig. 1A, B, arrows, and video 1 of the supplementary data), which also showed radiological findings of right ventricle (RV) overload and dysfunction. The echocardiogram showed findings of massive PE and a large floating thrombus extending from the RV inflow tract to the main pulmonary artery (Fig. 1C–F, arrows, and video 2 of the supplementary data). Initial PESI (Pulmonary Embolism Severity Index) score was 137, suggesting high-risk 30-day mortality. Although the patient was haemodynamic stable, taking into account the large thrombotic burden and the risk of thrombus fragmentation with additional re-embolism, urgent surgical embolectomy was indicated.
The patient underwent cardiac surgery, during which multiple thrombi were removed from the right atrium, RV, and both pulmonary arteries (Fig. 1G). During post-surgery period the patient suffered a cardiogenic shock due to RV dysfunction that required vasoactive drug support and a severe pulmonary haemorrhage, reperfusion related, that was managed conservatively. He was finally discharged 34 days after admission and assessed 4 weeks later in outpatient clinic with an adequate clinical situation, no residual pulmonary hypertension but persistent mild RV dysfunction.
This case depicts a life-threatening PE presentation called “thrombus-in-transit” that entails additional hazards and may require prompt interventions regardless of the initial assessment of PE severity and risk of early death.
FundingNo funding has been received for the publication of this article.
Authors’ contributionsAll authors have contributed equally to the conception, writing and critical review of this article and have given their final approval to the version that will be published.
Conflicts of interestNone of the authors have any conflict of interest to declare.